Height and weight were measured to the nearest 0.1 cm and 0.1 kg, respectively, with the subject standing barefoot in light clothes. Physical examination included anthropometric measurements, blood pressure, and medical history. Information regarding birthday, gender, and smoking status were collected. The health interview was performed by trained medical staff at community clinics using a well-established questionnaire to determine demographic and behavioral characteristics of the study population. 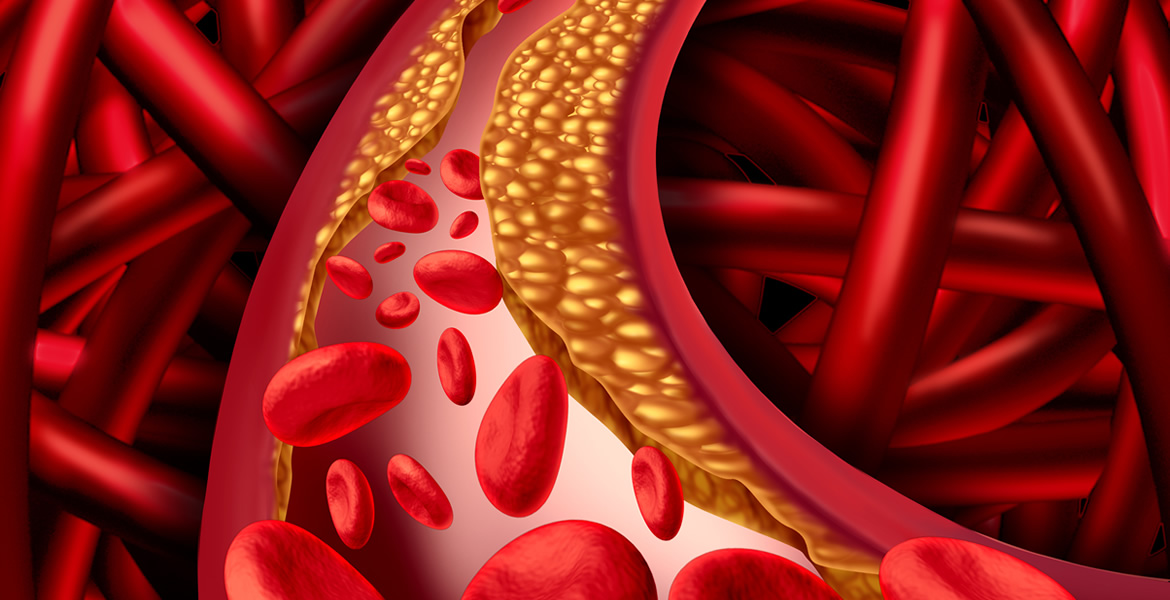
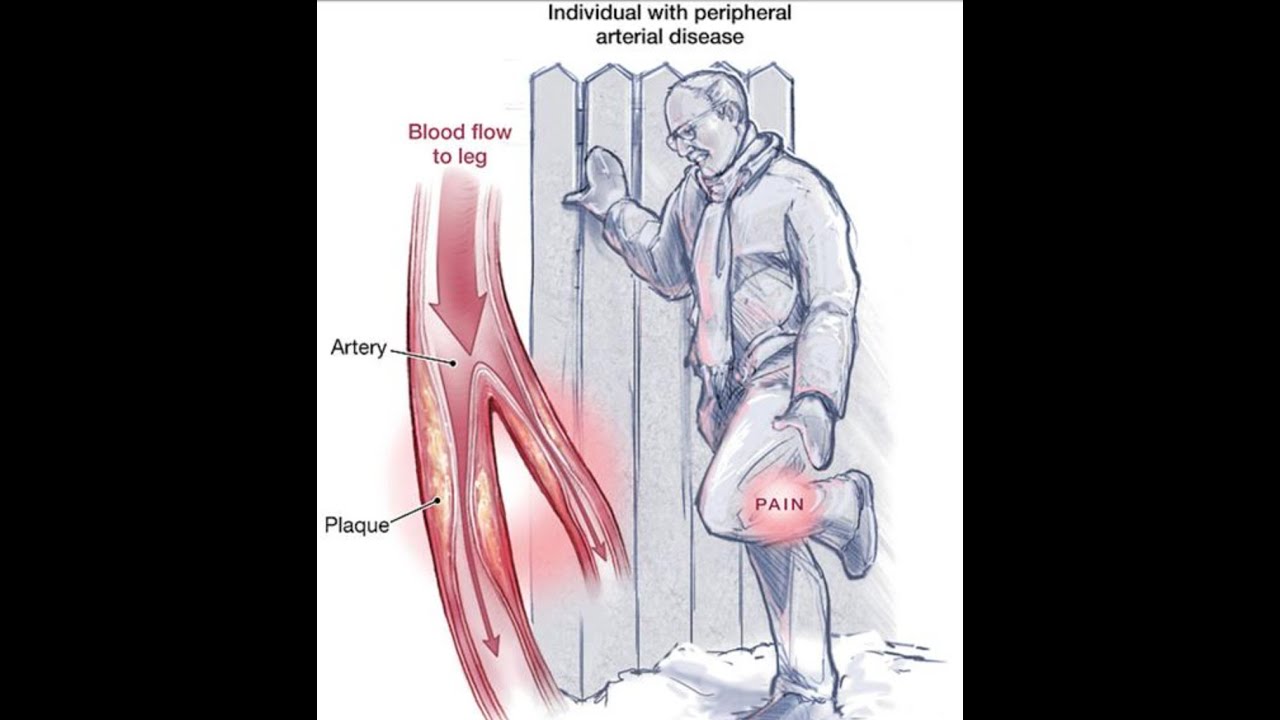
All participants provided written informed consent to attend this study and subsequent follow-up examination, and the study protocol and ethical approval was obtained from the Ethic Committee of Beijing Municipal Science and Technology Commission. Of the remaining participants, 164 had baseline PAD and 4 had missing data on core covariates the final analysis included 4,201 people who were free of PAD at baseline. During the 2-year follow-up duration, 1,095 participants emigrated or relocated, 402 refused to attend the follow-up examination, and 19 died. In brief, 5,885 participants from 38 communities were recruited. The present study included participants who were 50 years and over. A more detailed study design was described previously ( 13, 14). This study was a prospective cohort with participants originally recruited for chronic diseases and risk factors assessment in Beijing in 2007 with additional 2-year follow-up until 2009. Patients and Methods Study Design and Participants The present study aimed to examine the incidence of PAD, and to assess its association with pulse pressure in a general senior population. A prospective investigation of the association between pulse pressure and PAD remains scarce. However, most of these studies were based on cross-sectional design or case–control setting in which the temporal order was difficult to establish due to the weakness of study design. Previous investigations suggested higher pulse pressure may be an independent predictor for PAD and this relationship was observed in several studies ( 10– 12). Identification of those with PAD has profound public health and clinical implications for earlier disease prevention and treatment ( 5).Ī number of risk factors have been identified for PAD risk assessment, such as smoking, diabetes, height, and dyslipidemia ( 6– 9). It is also a strong predictor for cardiovascular diseases, mortality, and stroke, independent of traditional cardiovascular risk factors ( 3, 4). Peripheral arterial disease (PAD) is a common circulatory problem in which narrowed arteries reduce blood flow to limbs ( 1, 2). A linear trend was observed for the association of pulse pressure with PAD.Ĭonclusion: Higher pulse pressure was associated with higher PAD incidence. After adjusting for baseline age, sex, body mass index, hypertension, diabetes, total cholesterol, and high-density lipoprotein cholesterol, and smoking, the hazard ratio and 95% confidence interval for people with pulse pressure greater than 60 mmHg was 2.20 (1.53, 3.15) compared with those whose pulse pressure was less than 40 mmHg. Results: During a 2-year follow-up time, 357 of 4,201 (8.5%) participants developed PAD with 105 (6.9%) men and 252 (9.4%) women, respectively. Cox proportional hazard regression model was used to quantify the magnitude of pulse pressure on PAD incidence. PAD was defined as an ankle brachial index value <0.9 in either leg. Methods: We utilized data from a cohort conducted in Beijing with additionally 2-year follow-up time. This study aimed to investigate the association of pulse pressure with PAD incidence in an elderly general population.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
